General Gynecologic Care
General Gynecology
We provide complete gynecological care for patients from childhood through menopause. Each life stage brings bodily changes and varying needs. Our primary purpose is to empower women to take a proactive approach to their health care by educating and informing. The annual well woman exam is an essential part of preventative care. Beyond routine exams, our board-certified physicians treat a variety of complex conditions associated with the female reproductive system.
Abnormal Bleeding
Abnormal bleeding is defined as erratic or excessive vaginal bleeding. Signs include a heavy period, bleeding between periods/after sex, or during menopause, very long periods, or irregular periods. It is most common when menstruation begins and during the years prior to menopause. Hormone imbalances are often to blame. Other causes may be structural abnormalities in the uterus, precancer or cancer, infections, medical conditions like kidney or pelvic inflammation, and medications.
Endometriosis/Pelvic Pain
Endometriosis is a disease in which the endometrium (the tissue that lines the inside of the uterus) is present outside of the uterus. It most commonly occurs in the lower abdomen or pelvis. Symptoms include lower abdominal pain, pain with menstrual periods, pain with sexual intercourse, and difficulty getting pregnant. Conversely, some women with endometriosis may not have any symptoms. Symptoms can be constant or cyclical, worsening before or during a period.
Infections
Bladder
Bladder infections are the most common type of urinary tract infection (UTI), but any part of the urinary tract can become infected – the urethra, bladder, ureters, and kidneys. Most infections are caused by bacteria from the bowel reaching the urethra and bladder. Symptoms include a burning feeling when urinating, a strong and persistent urge to urinate, pink or red urine, releasing small amounts of urine, and strong-smelling urine.
Vaginal
Vaginal infections are due to an imbalance of yeast and bacteria that normally live in the vagina. Vaginal discharge is usually clear or slightly cloudy and doesn’t smell or itch. An infection may be present if the discharge changes color, is heavier, or smells different. There may also be itching, burning, swelling or soreness around or outside the vagina, burning with urination, or uncomfortable sexual intercourse.
Menopause
Perimenopause
Perimenopause occurs several years before menopause when the ovaries make less estrogen. It usually starts in women’s 40’s, but it can take place in the 30’s or earlier. Symptoms include hot flashes, breast tenderness, worsened PMS, lower sex drive, fatigue, irregular periods, vaginal dryness/discomfort during sex, urine leakage when coughing or sneezing, urinary urgency, mood swings, dry skin/eyes/mouth, and sleep troubles. Irregular periods are common and normal during this phase.
Menopause
Menopause is when the ovaries no longer release an egg every month and menstruation stops, marking the end of the reproductive years. It is a regular part of aging, typically after the age of 40. Most will experience hot flashes, sudden feelings of warmth spreading over the body, which range from mild in most women to severe in others. Symptoms include all the perimenopausal ones listed.
Post-menopause
During post-menopause, symptoms experienced during the earlier stages may stop. Post-menopausal vaginal bleeding should not occur, so it is important to see an OB/GYN if detected. The estrogen decrease associated with post-menopause impacts other body systems. There can be an increase in heart disease, bone loss, bladder issues such as leakage or infections, reduced vaginal lubrication or atrophy, and lower metabolic rate.
Hormone Replacement Therapy
Hormone replacement therapy (HRT) is an option to combat the increased health risks or discomforts of post-menopause. HRT may relieve hot flashes, night sweats, vaginal dryness, and protect against bone loss. However, it may also increase risk of breast and uterine cancer, stroke, heart disease, deep vein thrombosis, and gall bladder disease. Hormones are available topically (patch, cream) or orally, and they can be bioidentical (plant-derived hormones) or traditional (lab-made or found in the urine of pregnant horses). Our OB/GYNs can determine which is best depending on each patient’s symptoms and medical history.
Menstruation
PMS Management
Premenstrual syndrome (PMS) is a group of changes that occur before a monthly cycle. Emotional signs are mood swings, irritability, depression, crying spells, and anxiety. Physical signs are joint or muscle pain, headache, fatigue, weight gain, bloating, tender breasts, acne, and appetite changes. Symptoms usually disappear within 4 days after the menstrual cycle has started. However, the emotional stress and physical pain can be debilitating for some. Causes can be hormonal fluctuations or fluctuations of serotonin in the brain.
Painful Periods
Pain associated with menstruation is called dysmenorrhea. Usually, the pain is mild. But, for some the pain is severe enough to impact daily life. Severe period pain can be accompanied by diarrhea, nausea, vomiting, headache, and dizziness. Medications are the first step to treating the pain, assuming a physical exam does not reveal other extenuating factors such as fibroids or endometriosis. Birth control methods that contain hormones might also be helpful.
Irregular Periods
As a rule, women under 45 are experiencing irregular periods if their cycle occurs more often than 21 days, less often than 35 days, or lasts longer than 7 days. Periods are also considered irregular if time between each period changes, there is more/less blood loss than usual, or the number of days of the period varies a lot. There are many causes, such as birth control pills, changing medications, over or underactive thyroid, hormonal changes, uterine polyps or fibroids, endometriosis, pelvic inflammatory disease, polycystic ovary syndrome, premature ovarian insufficiency, and stress or lifestyle. It is normal to have irregular periods for the first few years of menstruation and during perimenopause.
Ovarian Cysts
Ovarian cysts are fluid-filled sacs in an ovary or on its surface. Ovarian cysts can form at any time. Most are harmless, have no symptoms, and disappear without treatment in a few months. However, they can cause serious symptoms, especially when ruptured. A large ovarian cyst can cause pelvic pain, fullness in the abdomen, or bloating. Regular well-woman pelvic exams can detect ovarian cysts and circumvent problems.
PCOS
Polycystic ovary syndrome (PCOS) occurs when the ovaries produce an abnormal amount of androgens or male sex hormones. Numerous small fluid-filled sacs or cysts form in the ovaries. PCOS impacts women from 15 – 44 during their child-bearing years. Since PCOS is characterized by excess male hormones, symptoms include missed menstrual periods and difficulty getting pregnant. The hormones can also cause hair growth on the face and body or, conversely, baldness.
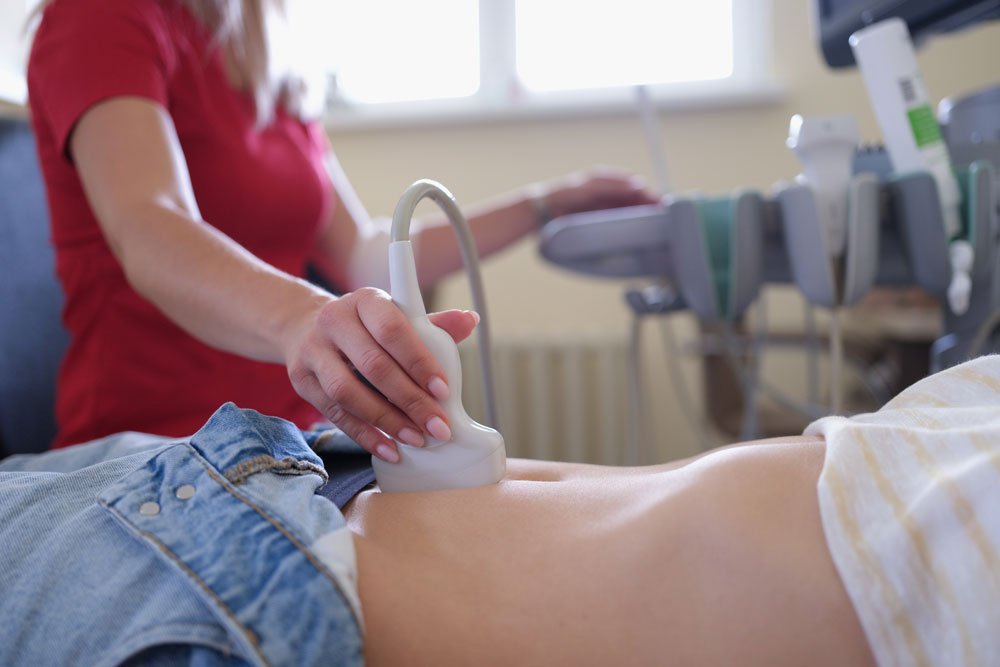
Pelvic Ultrasound
A pelvic ultrasound produces images of the female pelvic organs and structures within the uterus, cervix, vagina, fallopian tubes, and ovaries. It is used as a diagnostic tool. It is safe and painless because the test uses sound waves to make the images, called sonograms. A pelvic ultrasound might be recommended for those having difficulty getting pregnant, pain during sex, pain during urination, pelvic or abdominal pain, swelling in the abdomen, unusual periods, bleeding after menopause, or urinary incontinence (leakage).
Polyps
Cervical
Cervical polyps are fingerlike growths on the cervical canal, the pathway connecting the uterus to the vagina. They originate from the mucosal surface of the cervix and are reddish, purplish, or grayish. Cervical polyps are relatively common and mostly benign. Symptoms might include heavier than normal periods, bleeding after sex, bleeding between periods, vaginal discharge, or bleeding after menopause. Normally they are found during a Pap test so regular annual well-woman checks are recommended.
Endometrial
Endometrial polyps are small, soft growths that result from an overgrowth of cells in the lining of the uterus (endometrium). Size ranges from a small seed to a golf ball. They are more common in women 40 – 60, perhaps due to the changes in estrogen levels before and during menopause. Obesity, high blood pressure, and the breast cancer drug tamoxifen create higher risk. Symptoms include irregular periods, heavy periods, bleeding or spotting between periods, vaginal bleeding after menopause, and trouble getting pregnant. Most polyps are benign but can turn into cancer later which is why annual well-woman exams are important.
Uterus Abnormalities/Fibroids
Structural irregularities of the uterus can contribute to infertility, recurrent miscarriage, or complications during delivery. They can be congenital or acquired. Congenital abnormalities include septate (partitioned by the septum wall), bicornuate (divided into two spaces), unicornuate (half a uterus), and didelphys (double uterine cavities with their own cervix). Fibroids are noncancerous muscle growths in the uterus that also impact fertility. They can become large enough to obstruct the embryo from implanting on the uterine lining. These uterine issues are typically diagnosed during a pelvic exam and imaging tests.
Urology (General)
Bladder/Urinary Infections
A urinary tract infection (UTI) can occur in any part of the urinary system – kidneys, ureters, bladder, or urethra. Most involve the lower urinary tract (bladder, urethra). These infections can be painful and can lead to serious consequences if spreading to the kidneys. Symptoms include a strong or persistent urge to urinate, burning during urination, passing frequent yet small amounts, cloudy urine, blood or strong odor in urine, or pelvic pain.
Incontinence
Urinary incontinence is the loss of bladder control. It can range from occasionally leaking urine, for example during a cough or laugh or when exercising, to not reaching a toilet in time when feeling a strong urge to urinate. Incontinence is more likely among pregnant women, following childbirth, older women, being overweight, after menopause, and other more serious health conditions.
Well Woman Care
The well-woman exam is a comprehensive annual checkup that screens for sexual and reproductive health. It is a time when our OB/GYNs can discuss the overall health and well-being with a patient and recommend preventative services. The exam includes a medical history, breast and pelvic exam, necessary lab tests such as a Pap smear or check for sexually transmitted diseases (STDs), immunizations, and, for reproductive-aged women any medical testing and treatments to align with future plans. These exams are essential to catch early signs of cancer and other health problems. The American College of Obstetricians and Gynecologists (ACOG) recommends that girls should first see a gynecologist between the ages of 13 and 15, although most girls will not need a pelvic exam on that first visit.

